How NHS Private Patient Units are Helping Fight the Pandemic
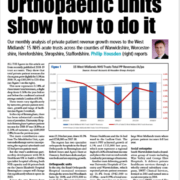
Our last update reported on the upbeat messages flowing from the NHS PPUs Annual Conference, including an estimate of 9% growth for the year ending March 2020 to £700m revenues, together with a forecast of 10% further growth for 2020/21.
How quickly things can change…
In May, Philip Housden’s column in the Independent Practitioner Today Magazine, focused on COVID-19 and the contribution private patient units are making within the NHS to the national combined effort:

Since the decision was taken to suspend private activity within the NHS and to use PPU beds for coronavirus capacity in mid-March, services right across the country have been redirected to other uses. This has included alternative uses for single ensuite patient rooms, rehousing non-COVID patients, and the transferring of clinical and non-clinical staff to other duties. There has been innovation too as the following updates demonstrate. These are a snapshot of the range of positive activity taking place right across the PPU sector right now.
First, London. London North West University Healthcare NHS Trust was one of the first Trusts in the country to receive high numbers of coronavirus patients. In response, it was decided at the beginning of March to transition the private patient unit, St Marks Private Healthcare, and allow its staff and single ensuite rooms to be used in the care of NHS patients.
David A Osborne, Head of Business Development at the Trust adds “The unit was initially used by patients awaiting the results of COVID-19 tests before being transferred to the appropriate hospital ward. However, the unit itself quickly became, and currently remains, a COVID-19 positive ward. The actions taken demonstrate how the private patient unit has quickly and effectively responded to meet the needs of COVID-19 patients, the NHS, and the local community.”
At Royal National Orthopaedic Hospital, Stanmore the Private Care Ward has become the Trust’s Respiratory Ward for COVID 19 positive patients, primarily due to the single room layout. The ward is being staffed by PPU staff supported by the wider Trust. Private patients that fall into one of six protected pathways, including cancer, spinal cord injuries, bone infections, and urgent cases are being admitted onto NHS wards but there are no elective surgery admissions outside the protected pathways. Eileen Scrase, Head of Private Care said “In this time of uncertainty as we all grapple with the greatest challenge of a generation I am deeply humbled and very proud of all of the staff for the work they are doing.”
The Royal Marsden is safely treating all patients, ensuring cancer treatment can continue whilst managing those patients who have also been diagnosed with COVID-19 which can be very concerning for immune-suppressed patients.
During the current situation, the private inpatient areas at The Royal Marsden have been identified on both sites as wards in which to cohort COVID-19 positive cancer patients due to their layout and location in the hospitals.
Shams Maladwala said: “We have also been leading a ‘cancer surgery hub’ in collaboration with University College London Hospital and Guy’s and St Thomas’ and private providers, to co-ordinate cancer services across London to ensure that patients continue to receive the surgical treatment they require during the COVID-19 pandemic. This will maximise available capacity and expertise to relieve the pressure management of the COVID-19 pandemic places on the NHS.”
Across the capital, it is a similar story. At Guy’s and St Thomas, all facilities have currently been handed over to NHS services to support the COVID response and generally speaking, Trusts have given over the PPU beds to NHS needs and the clinical staff are caring for NHS patients
Turning to the South East, Portsmouth Hospitals Trust’s PPU, 13 bed Harbour Suite, was originally designed as an ‘Infectious Disease’ ward, with negative pressure single ensuite rooms (negative pressure rooms significantly reduce the risks associated with aerosol-generating procedures – AGP) and this meant the PPU was perfectly set up to take COVID-19 patients who are critically ill and requiring Non-Invasive Ventilation (NIV). The floor layout has enabled an increase in beds to 20 with a move of other services that had been co-located.
Steve Thomas, Divisional Nurse Director – Surgery & Outpatients, (including private patients) said, “PPU staff, due to their work with bariatric patients and the range of private patients they would care for with extended comorbidities are highly skilled in looking for early signs of the deteriorating patient. They are central to the Trust response and work closely with the respiratory clinicians and nursing teams are also now based on the PPU ward and support 24/7. Our PPU is the Trust front line ward for NIV patients and the staff have all done incredibly well and are proving to the whole Trust they are an amazing team.”
At Epsom and St Helier Romi Appanah, Head of Private Patients confirmed that the 20 bed Northey Suite was chosen to cohort COVID-19 suspected or positive patients. From the 13th of March, the unit stopped all private activities. A few private inpatients who were not ready for discharge at the time were moved into single rooms to another ‘clean’ surgical ward until they were discharged. The PPU nursing staff remained on the Northey Suite to take care of the NHS patients. Since then several other wards were needed to cohort the surge of COVID-19 suspected or confirmed patients and the Northey Suite was then declared a low acuity COVID-19 area. There was a reduction in A&E attendance and this combined with nursing staff shortage resulted in the Northey Suite being closed temporarily, with PPU nursing staff caring for patients on other wards. The administrative staff were working from home and assisting with other admin duties around the hospital, including covering ward clerking duties.
The same approach has been taken across Sussex PPUs. In East Sussex, the 16-bed Michelham Unit at Eastbourne General Hospital has closed and is being used as a cohort area for potential COVID 19 patients. In Western Sussex Hospitals both the 16 bed Chichester Suite at Chichester and the 5-bed Downlands Suite at Worthing Hospital are also closed for private patients with resources available for COVID-19 demand.
In the South West, Sarah Porter, Private & Overseas Patient Manager for Somerset NHS FT told IPT that the Parkside Unit PPU is currently being used for surgery (mainly vascular) that is still being admitted to the hospital. However, all private patient work is closed down in the Trust for the foreseeable future. Here too, administrative staff have all been redeployed to COVID projects, including 3 members co-ordinating the accommodation for staff that want to or need to isolate away from family members, and also the set-up of a pop-up shop for staff.
Gloucestershire Hospitals is still offering a limited service to private patients, including chemotherapy and urgent cardiology cases. Here too, some staff have been redeployed.
In East Anglia, the 8-bed Charnwood Suite at James Paget Hospital, Great Yarmouth has been closed but as all of the rooms are en-suite it is being used as a showering/changing facility for the wider hospital staff. The PPU staff are all redeployed into other areas and the equipment and stock on the ward is also supporting the Trust. Also, the 4 consulting roomed private patient outpatient clinic is closed and has been made available to the team who have implemented remote consultations.
In the Midlands, at South Warwickshire NHS FT, Pauline Salmon, interim clinic manager, confirmed that The Grafton Suite at Stratford Hospital saw its last private patient on 18th March. The clinic space of two treatment rooms, three consulting rooms, and ophthalmic rooms is now re-housing the oncology department from Warwick Hospital, which in turn has enabled that separate building at the front of the hospital to become a COVID- 19 reception location.
Finally, in the north of England, Newcastle upon Tyne Hospitals have closed their 5 bed Park Suite to private activity with the nursing staff supporting colleagues in other units during the crisis period.
Similarly, Harrogate and District NHS FT has temporarily suspended services out of the 10 bed Harrogate Harlow unit. This is to enable clinical and administrative teams to support the wider Trust at Harrogate District Hospital. Beth Barron, Operational Director Elective Care, and manager of the private patient services has joined the Trust’s Incident Co-ordination Centre, which has been supporting the set-up of the new NHS Nightingale Yorkshire and Humber hospital at Harrogate Convention Centre, which was officially opened on 21 April by Captain Tom Moore.
There is a great deal of opportunity – as well as risk – to the sector in the coming months. Clearly, the 2020/21 financial forecasts are going to be missed, costing the NHS approximately £60m a month. Many managers have shared how they expect PPU services to be different when private practice is reinstated. As this round-up has demonstrated, these managers and their teams now have many positive examples to share with CEOs and Exec Teams about the valuable contribution that PPUs play within the wider NHS. Private patient units provide over 1,200 beds, and the revenues enable the employment of several thousand staff –capacity and skills that wouldn’t be there if PPUs were not making a surplus.
However, only Trusts with PPUs have had the benefit of these flexible resources, able to be re-purposed for the crisis. It’s not clear when these resources will be returned to support private care. But when they do they will be needed as there will be a great deal of pent-up demand for healthcare, and with waiting lists and access times at all-time highs, demand for private healthcare will be strong. The crisis has demonstrated the value of 24/7 critical care back up – and this too may lead to a greater understanding of the Patient Safety benefits of private care in the NHS setting – and an expansion of PPUs into many more Trusts.